What are facet joint injections?
Facet joints are small joints on both sides of your spine that connect adjacent vertebrae and help guide movement. When these joints become inflamed or arthritic, they can cause persistent neck or lower back pain, usually felt as a dull, aching sensation along the spine rather than radiating pain down your arm or leg.
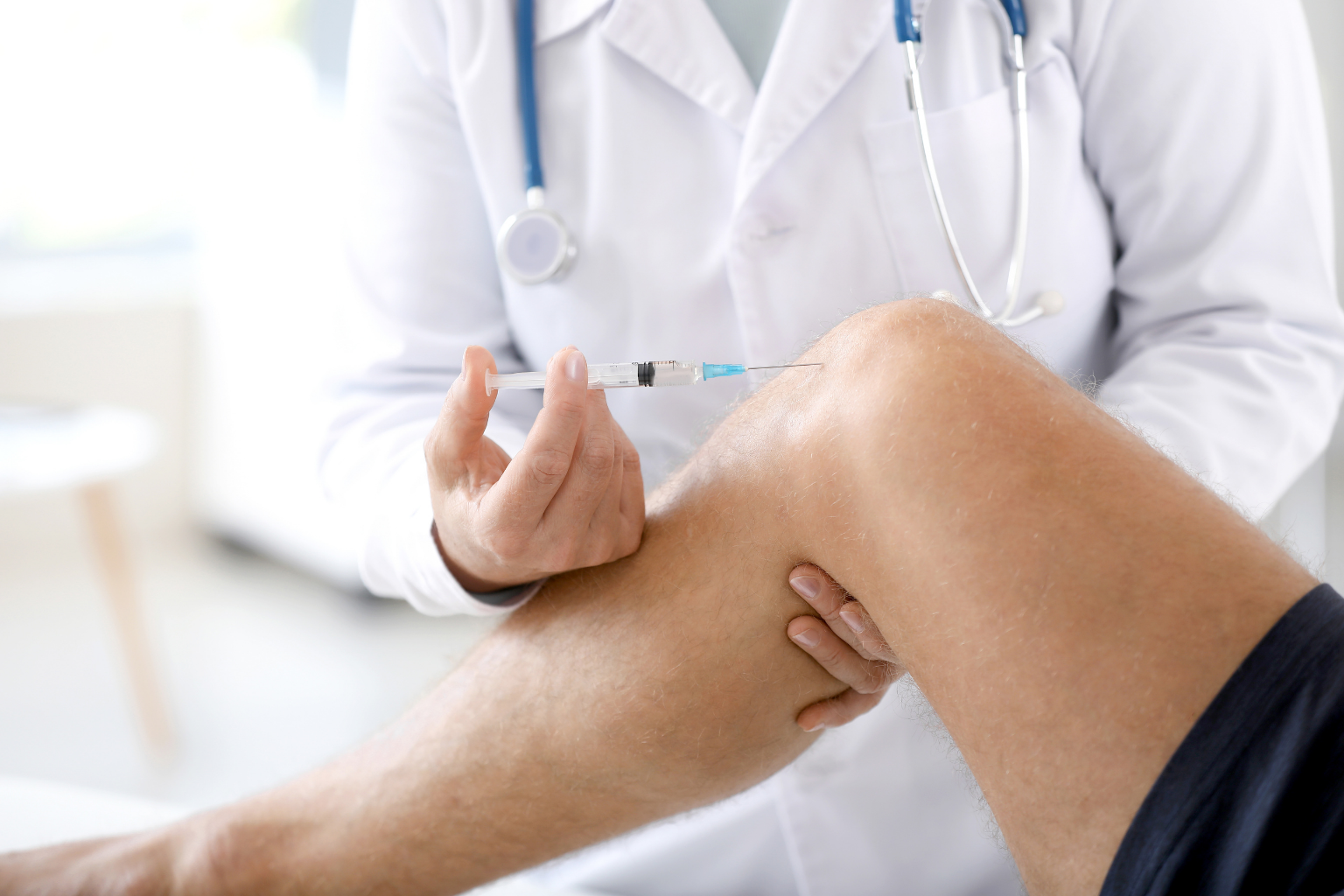
Facet joint injections address this pain by delivering a corticosteroid (an anti-inflammatory medication) and a local anesthetic directly into the affected joint under ultrasound visualisation. The medication reduces inflammation and pain, often enabling you to move more comfortably and engage in physiotherapy or rehabilitation. The injection is not a cure for arthritis or degenerative changes, but rather symptom relief that supports your recovery and function.
Conditions where they help
Facet joint osteoarthritis
Wear and tear on facet joints creates localised stiffness and pain, particularly when extending your neck or back. Injections can provide weeks to months of relief, allowing you to resume activities.
Mechanical low back pain
Pain centred in your lower back without radiation into your leg may stem from facet joint strain or inflammation. This responds well to injections, especially when combined with physiotherapy addressing posture and movement patterns.
Cervical facet joint syndrome
Neck pain from facet joint problems often worsens with certain head movements. Ultrasound-guided injection at the affected level can restore a better range of motion.
Post-injury facet pain
After whiplash or other spinal trauma, facet joints may become inflamed. Early injection can interrupt the pain cycle and support healing.
Failed back surgery syndrome
Some patients experience persistent facet-mediated pain after spinal surgery. Injections can be particularly helpful in these cases.
Symptoms to watch for
- Localised neck or lower back pain, often worse with extension or rotation
- Stiffness that improves with movement or bending forward
- Pain that does not radiate significantly into your arm or leg
- Discomfort centred along the midline of your spine
- Symptoms worse at the end of the day or after prolonged standing
When to see a doctor
If your back or neck pain is affecting daily activities such as working, exercising, or sleeping, you should see your GP or a specialist to confirm the source of your pain. A clinician will perform a physical examination and review imaging (such as X-rays or MRI) to determine whether facet joints are likely causing your symptoms. Not all back pain originates from facet joints, so accurate diagnosis is essential before pursuing an injection.
You should seek urgent medical assessment if you experience new numbness or weakness in your legs, loss of bowel or bladder control, fever, or pain that worsens sharply after an injection. For genuine emergencies such as severe neurological deterioration, attend A&E or call 999.
If back or neck pain is affecting your daily life, our doctors at Saba Health Clinic can help you find answers and a treatment plan that fits you. Same-day and next-day appointments are available.
What to expect
Facet joint injections are typically part of a broader pain management strategy. Conservative treatments such as physiotherapy, activity modification, and anti-inflammatory medicines are tried first. If these provide insufficient relief and imaging shows facet joint changes, injection therapy becomes appropriate. For patients who benefit temporarily from injections but experience recurring pain, radiofrequency ablation (a procedure that disables pain nerves) may offer longer-lasting relief.
Before the procedure
Your clinician will review your medical history, current medications (especially blood-thinners), and imaging studies to plan the injection. You’ll discuss the expected benefits, potential risks, and alternatives. If you’re taking anticoagulants such as warfarin or apixaban, your clinician will advise whether these need adjustment beforehand.
During the procedure
You’ll be positioned to allow safe access to the affected facet joint, prone (face down) for lumbar injections or sitting for cervical ones. The clinician will scan the area with ultrasound to confirm anatomy, plan the needle path, and identify structures to avoid. The skin is cleansed thoroughly with an antiseptic, then a small-gauge needle is advanced under live ultrasound visualisation toward the target joint. Once correctly positioned, a small volume of corticosteroid and local anesthetic (typically 0.5-1.5 mL) is injected slowly into the joint space. The entire procedure usually takes 15-25 minutes, though total clinic time, including preparation and observation, extends longer.
Most patients experience only mild to moderate discomfort, a brief stinging as the needle enters the skin, mild pressure as it advances deeper, and a sensation of fullness as medication enters the small joint. Significant pain is uncommon; if it occurs, tell your clinician immediately, as this may indicate the need for position adjustment.
Immediately after
The local anesthetic provides immediate pain relief lasting 2-6 hours. You’ll rest in the waiting room for 20-30 minutes to ensure no dizziness or adverse reaction. During this period, the injected area may feel numb; avoid stressing that part of your spine, as the numbness masks pain that normally prevents overloading. You can resume normal activity after this observation window, but avoid strenuous activities, heavy lifting, or aggravating movements for 24-48 hours.
What happens next
As the local anesthetic wears off (after a few hours), your pain may return briefly before the corticosteroid begins reducing inflammation. Some patients experience a temporary pain increase (steroid flare) for 24-72 hours. This is a normal inflammatory response and resolves with rest, ice, and paracetamol if needed. Most people notice meaningful improvement during days 3-14, with maximum benefit typically by weeks 2-6. If no improvement is evident by 2-3 weeks, substantial delayed benefit is unlikely.
During this early recovery window, physiotherapy or rehabilitation becomes especially valuable, as reduced pain allows more effective exercise and movement retraining. Gradually increase activity as symptoms improve, but avoid returning suddenly to movements that previously triggered pain.
Recovery and prevention
Benefit duration varies considerably. Some patients achieve relief lasting several weeks; others experience months of improvement. Factors influencing longevity include the severity of underlying arthritis, ongoing mechanical stress, adherence to activity modification, and engagement in physiotherapy.
Repeat injections are sometimes appropriate if symptoms recur after an initial good response. Guidelines recommend limiting injections to 3-4 per year per spinal region, with at least 2-3 months between injections, to minimise cumulative steroid exposure. If benefits consistently recur after weeks rather than months, radiofrequency ablation may be worth considering, as it can provide 6-12 months or longer of relief for appropriately selected patients.
To extend your results, continue physiotherapy addressing posture, core strength, and movement mechanics. Avoid prolonged static positions, maintain good lifting technique, and take regular breaks from sitting or standing.
SABA Health Clinic
Chapel House, Thremhall Park, Bishop's Stortford, Hertfordshire CM22 7WE
Phone: 01279 874388
WhatsApp: +44 7703 980989
Email: contact@sabahealth.co.uk

.png)




